What treatments are possible?
Wound care is based on three elements that make up what is known as the “VIP” approach. These three elements play an important role in healing a persistent wound. For example, even a small sore on a foot with poor blood circulation can become a serious problem if it is not treated quickly.
In addition to VIP treatments, the wound requires special care to help it heal.
Treatments for diabetic foot in the presence of a wound
The VIP approach to treatment:
- V Vascular: ensure good blood circulation;
- I Infection: control the infection;
- P Pressure: avoid all pressure on the foot.
Wound care:
- debridement of the wound;
- dressings.
Ensure good blood circulation
When a wound develops on a diabetic foot, it is important to make sure that there is sufficient blood supply to the foot. If this is not the case, there are ways to improve blood flow, including:
- dilation of blocked vessels via a procedure known as percutaneous angioplasty;
- a bypass, which involves creating a bridge to allow the blood to get around the blockage.
In some cases, it is necessary to perform both procedures. The goal is to restore blood supply to the foot so that oxygen and nutrients can reach the wound, allowing it to heal and reducing the risk of amputation.
Control the infection
People suffering from diabetes often have had hyperglycemia for a long time. When the level of sugar in your blood is high over a lengthy period, your immune system becomes weaker and less effective at fighting infection.
Initially, the signs may not be very noticeable, even if the infection is severe. Watch for changes in temperature, heat, redness, discharge or pain, as mentioned in the section on Complications.
We encourage you to inspect your feet daily and to see a health care professional promptly if you notice any changes. The main challenge for the health care team will be to determine which microbe(s), also known as germs or bacteria, are responsible for your infection, so they can prescribe the right antibiotic.
If the medication is in tablet form, you will take it orally (by mouth). If not, it will be given through a device that delivers it directly to your veins. A course of antibiotics lasts about seven to 14 days. It may be necessary to extend the treatment for several weeks if the bones are affected or if there is a risk of amputation.
Relieve pressure on the foot through offloading
Many of the treatments used to promote wound healing require your cooperation. This is the case with “offloading,” which in medical terms refers to the different methods of removing all forms of pressure on the foot.
For the wound to heal, pressure on the foot must be reduced at all times, including pressure created by your body weight. “At all times” means 24 hours a day, seven days a week, and not a minute less. If your health professional prescribes a wound offloading treatment, you must stick to it at all times. The importance of this cannot be overstated.
In fact, the offloading treatment you are prescribed to heal a diabetic plantar ulcer is the same type of treatment that would be recommended if you had suffered a foot fracture and were instructed to keep weight off the affected foot. Would you walk around on a fractured foot without wearing a cast? Obviously not. It is exactly the same for offloading a diabetic foot.
There are several types of devices and techniques associated with offloading. Some of them can be removed, while others cannot.
Removable offloading devices
These include offloading shoes or boots that can be put on and taken off. When used as prescribed, they can promote healing of the wound. Their main disadvantage is that they can be removed by the patient, who may then walk on the wound and in this way compromise healing.
The discharge boot with inflatable membrane is often prescribed for the discharge of UPDs.

Different types of forefoot or rearfoot offload shoes are often used to offload UPDs.
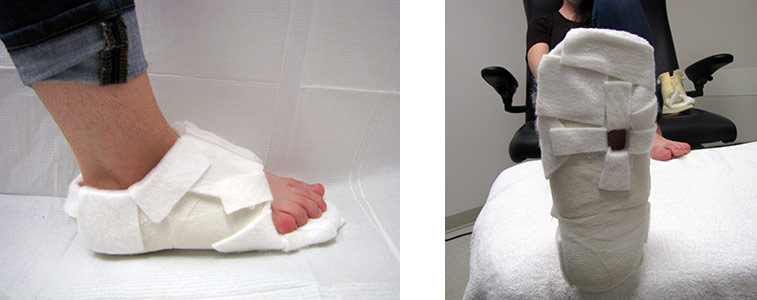
Certain custom-made offloading methods, such as this cast slipper from Ransart, are sometimes used in specialized centers for the management of the diabetic foot.
Photos: S. Hains
Non-removable casting devices
This type of gear is “irremovable.” The most effective device is a cast, similar to the cast that would be applied to treat a fracture. Called a total contact cast, this type of device cannot be removed. It is lightweight and painless, allowing you to remain mobile. It can considerably accelerate healing of the wound.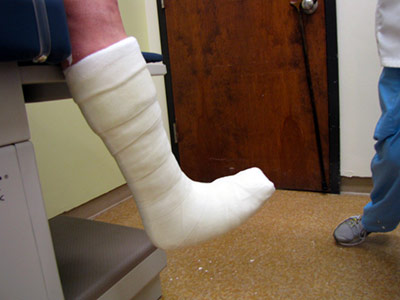
Total contact cast
Photo : S. Hains
Receive wound care and dressings
If you have a diabetic foot wound or ulcer, you should receive what is called “wound care.” This involves cleaning the wound, debriding it if necessary and applying a dressing. This care is provided by health professionals. Sometimes specialized dressings or other advanced wound care techniques will be used. It is important that you follow the recommendations made by the health professional to maximize your chances of recovery.
Debride the wound
The process of debriding a wound involves removing the necrotic tissue in and around the wound. This tissue is dead and it promotes infection and prevents the wound from healing. Debridement removes some of the bacteria that cause infection. By “cleaning out” the wound, it helps healthy tissue to heal.
Several methods of debridement are used, including dressings, drugs and scalpels or blades. Debridement should be combined with offloading to take pressure off the wound. This treatment is not painful.