Complications
What are the complications associated with diabetic foot?
Diabetic foot can lead to several complications, including an ulcer, which is a wound that does not heal, as well as infection, necrosis or amputation.
Ulcer or wound
Wounds or sores (also called ulcers) may form on the feet or ankles. If you have a wound, you should look out for the following signs:
- a discharge of pus that becomes more abundant;
- pus that changes texture or colour;
- odours;
- pain;
- changes in the appearance of the wound.
If you notice any of these signs, it is important to report them to your health professional.
Infection
Diabetes makes it harder for your system to fight infection. This puts you at greater risk. Infections can be superficial, on the surface of the skin, or deep, extending to the muscles and bones. They can also spread and cause other infections such as cellulitis, lymphangitis, abscesses or osteitis, which is an infection of the bone. They can also enter the bloodstream and spread throughout the body, which is known as “septicemia.”
Be on the lookout for:
- new or increased pain;
- redness;
- a warm sensation;
- swollen foot;
- fever, chills and vomiting.
In addition to fever and chills, you may experience other symptoms or discomfort that affect your entire body, such as fatigue. It’s also important to remember that higher blood sugar levels can be a sign that an infection has taken hold.
Fortunately, there is a lot that you can do to prevent infection or help it heal. A section of this portal is dedicated to this subject.
Necrosis
Uncontrolled infection can lead to tissue death, especially when blood circulation is poor. This is called gangrene or necrosis. It’s important to mention, however, that just because there are blackened areas in a wound does not necessarily mean there is gangrene or necrosis. These conditions can be confirmed by a health professional.
Necrosis is caused by a lack of or insufficient blood supply to an infected area of a limb. If the tissue is severely damaged and treatment has failed or is not available, amputation may be considered. That is why it is important to take preventive measures.
There are several signs of poor circulation, including these symptoms:
- when lying down, you notice that one leg is much paler than the other;
- your leg or part of your leg becomes very red when your foot is down;
- your foot or leg feels cool or cold;
- you have less and less hair on your leg;
- your toenails grow thicker;
- you feel pain when your leg is raised.
By being alert to these signs, a person with diabetes may be able to obtain treatment early enough to avoid amputation down the road.
Amputation
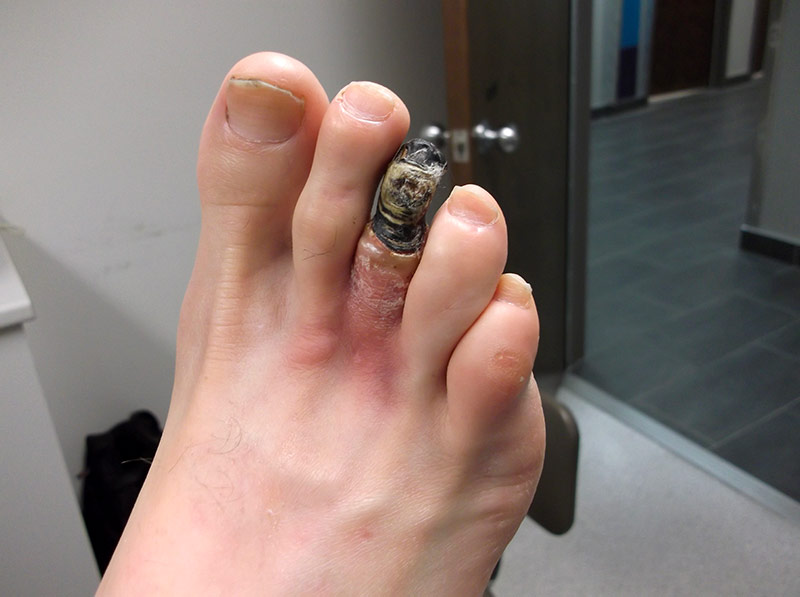
“Amputation” refers to surgery during which a limb or part of a limb is removed by a surgeon. In the case of diabetic foot, it is most often a toe or part of the foot or leg that is amputated, and rarely the entire limb. Amputation is considered as a last resort. It may be necessary if the blood circulation is insufficient, if there is severe infection or if treatment has failed.
Having an infection and peripheral arterial disease (PAD) at the same time increases the risk of amputation. Other conditions that can lead to amputation include:
- insufficient vascular supply and the presence of gangrene;
- uncontrollable or life-threatening infection (septicemia);
- a wound that won’t heal;
- intolerable pain.
An amputation will be performed only after every effort has been made to save the toe, foot or leg. This decision is made in consultation with the person affected and if it is in their best interest despite the undeniable impact on the quality of life going forward.
There are several treatments for peripheral arterial disease (PAD). These are discussed below.